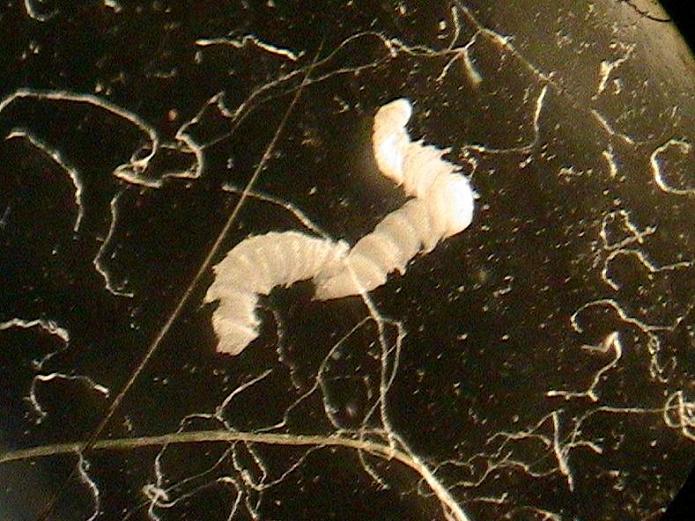
stercoralis in all patients who are to receive immunosuppressive therapy (especially corticosteroids and chemotherapy), as this can cause the hyperinfective syndrome. Doctors should consider infection with S. 4–7 Who is at risk?Īlthough history is important to identify those at risk of strongyloidiasis, the initial exposure to infective larvae may have occurred decades earlier. 3 In Australia, strongyloidiasis should be considered in residents of endemic areas, immigrants (including older patients from southern Europe), refugees, war veterans (World War II and Vietnam War), and workers and travellers returning from endemic areas with ‘a souvenir you don’t want to bring home’. 2 Some remote Aboriginal and Torres Strait Islander communities in Australia have had prevalences up to 60%. A prevalence greater than 5% is considered hyperendemic. 
1 Strongyloidiasis is endemic in tropical and subtropical regions of the world where warmth, moisture and poor sanitation favour its spread. EpidemiologyĪn estimated 370 million people worldwide are infected with S. Unless strongyloidiasis is deliberately considered, the diagnosis is unlikely to be made. General practitioners (GPs) have an important role in diagnosing and treating chronic strongyloidiasis to prevent cases of fatal hyperinfection. Chronic strongyloidiasis in humans is caused by the remarkably persistent roundworm Strongyloides stercoralis, distinguished by its unique autoinfective lifecycle.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
